Services
Gynecology

Birth Control
Birth Control Q & A
What are the best birth control options available now?
The best option depends on your lifestyle and your relationships with sexual partners. A 25-year-old single woman may have different needs than a 35-year-old married woman who is planning a family. Birth control pills remain one of the most common choices, and there are plenty of options within the category. There are two general types: mini-pills and combination pills. When selecting combination pills, there’s a further choice between conventional style or continuous dose pills. The conventional type follow the monthly cycle and users experience monthly menstrual periods. Continuous dosing may reduce periods to 4 per year or eliminate them completely. Long-acting reversible contraception (LARC) is another popular option.
What is LARC?
For a woman who’s made the decision to postpone childbearing for several years, choosing long-acting reversible contraception may be the ideal option. There are two choices:
Intrauterine devices, or IUDs, have been around the longest. IUDs works two ways: by creating conditions hostile to sperm to prevent fertilization, and by preventing an egg that does become fertilized from implanting in the uterine walls IUDs can be placed and removed during short appointments.
Contraceptive implants are thin plastic rods, about the size of a matchstick. These are implanted in the upper arm, and they work in much the same way as birth control pills. The implant typically lasts up to three years. While women who are done having children may choose LARCs, permanent sterilization is also an option.
What permanent sterilization options exist?
There are both surgical and non-surgical options for permanent sterilization:
Tubal ligation, commonly referred to as “having your tubes tied,” breaks the path of the fallopian tubes, preventing the egg and sperm from coming into contact. Surgery can now be done laparoscopically, reducing the invasiveness of the procedure.
Abnormal Pap Smears
Abnormal Pap Smears Q & A
What do “abnormal results” mean when it comes to a Pap smear?
Abnormal results on a Pap smear means that results came back positive. If you receive a negative result, everything is normal, and you don’t need to do anything. A positive result, however, doesn’t mean you have cervical cancer. The result depends on what the abnormality is.
What happens if I receive a false-negative test?
There’s really no way to know a false-negative test has occurred without re-testing. A false-negative result doesn’t happen because of a mistake in testing. It may be the result of an inadequate collection of cells during the Pap smear, a very small number of abnormal cells, or other cells that block the appearance of any abnormal cells. Given the slow rate at which cervical cancer develops, though, even if you have a false-negative result, it’s likely your next Pap smear will detect the abnormalities.
What are common abnormal results?
Atypical squamous cells of undetermined significance – or ASCUS. This means there are some abnormal squamous cells, but that, on its own, is not necessarily a problem. Further tests will check for other high cancer risk viruses. If there are no high-risk viruses present, then the abnormal cells aren’t a problem.
Squamous intraepithelial lesions will create abnormal results. Low grade changes mean that if there’s a lesion present, it’s years away from developing into cancer. More frequent Pap tests may be suggested, but you’re in no immediate danger. High grade changes mean that a lesion may become cancerous sooner, and more testing is required.
Atypical glandular cells will trigger an abnormal Pap smear, but only further testing can determine if the condition is cancerous. That testing determines the source and significance of the atypical cells.
Squamous cell cancer or adenocarcinoma cells do indicate that cancer is likely, and additional testing will likely be done immediately. Biopsies and colposcopies are typically performed in this case.

Menopause
Birth Control Q & A
What are the best birth control options available now?
The best option depends on your lifestyle and your relationships with sexual partners. A 25-year-old single woman may have different needs than a 35-year-old married woman who is planning a family. Birth control pills remain one of the most common choices, and there are plenty of options within the category. There are two general types: mini-pills and combination pills. When selecting combination pills, there’s a further choice between conventional style or continuous dose pills. The conventional type follow the monthly cycle and users experience monthly menstrual periods. Continuous dosing may reduce periods to 4 per year or eliminate them completely. Long-acting reversible contraception (LARC) is another popular option.
What is LARC?
For a woman who’s made the decision to postpone childbearing for several years, choosing long-acting reversible contraception may be the ideal option. There are two choices:
Intrauterine devices, or IUDs, have been around the longest. IUDs works two ways: by creating conditions hostile to sperm to prevent fertilization, and by preventing an egg that does become fertilized from implanting in the uterine walls IUDs can be placed and removed during short appointments.
Contraceptive implants are thin plastic rods, about the size of a matchstick. These are implanted in the upper arm, and they work in much the same way as birth control pills. The implant typically lasts up to three years. While women who are done having children may choose LARCs, permanent sterilization is also an option.
What permanent sterilization options exist?
There are both surgical and non-surgical options for permanent sterilization:
Tubal ligation, commonly referred to as “having your tubes tied,” breaks the path of the fallopian tubes, preventing the egg and sperm from coming into contact. Surgery can now be done laparoscopically, reducing the invasiveness of the procedure.

PCOS
PCOS Q & A
What causes PCOS?
The precise cause of PCOS isn’t known, but there are factors that seem to contribute to its development. There’s often a genetic link, and a patient with PCOS may have a mother or sister with the condition. Low-grade systemic infections stimulate polycystic activity in the ovaries. Patients with insulin resistance and an excess of insulin in the blood may also see an increased risk of PCOS. When ovaries are stimulated in any of these ways, production of male hormones rises, interfering with ovulation.
What are the symptoms of PCOS?
If a woman is susceptible to PCOS, symptoms typically start once she begins having menstrual periods. Occasionally, symptoms develop in later years, such as in response to a significant weight gain. Usually, two of the following symptoms may indicate PCOS:
Irregular periods: conditions such as menstrual intervals exceeding 35 days, less than 8 cycles per year, prolonged periods of either light or heavy flow, four months or longer without menstruating
High androgen levels: excess male hormones may create excess facial and body hair, male-pattern hair loss, and acne
Enlarged ovaries due to fluid-filled cysts surrounding eggs
PCOS usually affects each woman slightly differently, and the symptoms associated with PCOS are usually more severe with weight gain and obesity.
How is PCOS treated?
Treatment usually focuses on the predominant symptoms that a woman experiences, since these vary widely from case to case. Where weight is a factor, lifestyle changes to include increased physical activity and reduced calorie intake usually relieve symptoms. Even small changes in body weight may improve the patient’s condition.
It may help to regulate the menstrual cycle with medication, such as birth control pills that contain both estrogen and progestin and help decrease androgen production. Skin patches and vaginal rings may alternatively be prescribed. Progesterone therapy regulates the menstrual cycle, but doesn’t prevent pregnancy or reduce androgen levels. Excessive hair growth may also be treated as a separate condition.

Pelvic Pain
Pelvic Pain Q & A
What is pelvic pain and what other symptoms does it present?
Pelvic pain occurs anywhere between the hips and below the bellybutton. When it lasts longer than 6 months, whether continuously or intermittently, it’s referred to as chronic pelvic pain. It may be a condition on its own, a symptom of another disease, or it may occur as a cumulation of several conditions. Sometimes it’s difficult to identify a single cause for the pain.
The location of pain may not be focused, and may be felt through the pelvic region. Symptoms may be described as:
- Dull and aching or sharp and cramp-like pain
- Pain that’s steady and constant
- Pain that’s intermittent or varying
- Pressure deep within the pelvis area
- Pain occurring during intercourse, bowel movements, or urination
- Pain that’s aggravated by either sitting or standing for long periods, but usually relieved when lying down
What causes pelvic pain?
Usually, chronic pelvic pain is complex and it can have multiple causes. Other times it may be related to a single cause. Depression, emotional distress, and chronic stress are a few psychological factors that may contribute to pelvic pain. Physical causes may include:
- Endometriosis
- Tension in pelvic muscles
- Breakdown or straining of pelvic connective tissue
- Chronic pelvic inflammatory disease
- Ovarian cysts
- Fibroids
- Irritable bowel syndrome
- Interstitial cystitis
How is pelvic pain treated?
Doctors may prescribe medications to help ease pelvic pain. Over-the-counter or prescription pain relief may manage pain, but will provide little in the way of solving the problem. When pelvic pain seems tied to a woman’s menstrual cycle, hormone treatments may be effective. If infection is the source, antibiotics may clear up pelvic pain. Certain antidepressants have pain-relieving effects as well as mood-altering abilities, and these can sometimes reduce pelvic pain even in women without depression issues.
When specific points of origin for pelvic pain are identified, the doctor may inject long-acting, local anesthetics into those spots. Seeing a physical therapist for exercises and treatments may be effective in helping chronic pain stemming from soft tissue performance. If the doctor finds a problem that requires surgery, that may remove the source of the pain.

Endometrial Ablation
Endometrial Ablation Q & A
Why is endometrial ablation performed?
When heavy menstrual bleeding becomes a problem, there are typically medications that are tried first. These include birth control pills, patches, or vaginal rings, or intrauterine devices that also deliver hormones. When these fail to produce results, or when a patient can’t use these solutions, endometrial ablation becomes an option.
Endometrial ablation isn’t recommended for postmenopausal women or those with uterine abnormalities, cancer of the uterus, increased risk factors for uterine cancer, or those with active pelvic infections. Pregnancy can occur after endometrial ablation. However, since the uterine walls are deliberately damaged during the procedure, any pregnancy would be high-risk. Miscarriage may result as an effect of the ablation, or the pregnancy may be ectopic, which means it’s outside the uterus, typically in the fallopian tubes or cervix.
How is endometrial ablation performed?
The procedure may be performed in the office, depending on the method. Some methods require general anesthesia, and these are performed in a hospital. In most cases, the cervix must be widened to accept the ablation tool. This is done either with a series of rods, one after another, or using medication. Most ablation methods take 10 minutes or less and include:
- Cryoablation: extreme cold freezes and destroys the endometrium in a freeze cycle
- Electrosurgery: a scope with a heating element burns the endometrium
- Heated balloon: a balloon is inserted into the uterus then filled with hot fluid
- Hot fluid: heated saline is circulated in the uterus
- Microwave: a wand that emits microwaves heats and destroys the endometrium
- Radiofrequency: RF energy destroys endometrial tissue
What are the risks of endometrial ablation?
Complications from the procedure don’t occur often, but there are a few things to watch for, such as infection or excessive bleeding. Depending on the ablation method, other organs in the area may experience heat or cold damage. The uterine wall may also risk puncture from surgical instruments.

Endometriosis
Endometriosis Q & A
What causes endometriosis?
The exact cause of the condition isn’t known for certain, but several theories may explain how endometriosis happens. These include:
- Retrograde menstruation: uterine cells move back up the fallopian tubes, stick there, and start to grow
- Through a process called induction theory, certain cells may transform into uterine cells
- Scar implantation: uterine cells stick to the surgical scar tissue after C-sections or hysterectomies
- Lymphatic system transfer: cells from the uterus move to other locations through the lymph system
- Immune disorder: the body’s immune system may fail to recognize and remove endometrial cells growing outside the uterus.
What symptoms accompany endometriosis?
The main symptom of endometriosis is pelvic pain, usually associated with menstrual periods, but much more severe than typical menstrual pain. This pain may also increase over time. Symptoms of endometriosis include:
- Cramping and pain before, during and after the menstrual period
- Lower back and abdominal pain
- Pain during and after sex
- Pain accompanying urination or bowel movements, particularly during the menstrual period
- Excessive menstrual bleeding during and between periods
- Infertility: endometriosis is often first diagnosed when a woman seeks infertility treatment
- Fatigue, bloating, nausea, diarrhea, or constipation, particularly around menstrual periods
- The severity of endometriosis pain is not an indication of the advancement of the condition. Some women with advanced endometriosis have little pain. Others, with mild cases, may experience extreme pain.
How is endometriosis treated?
Treatment ranges from medication to surgery. Conservative treatments start the process, with surgery remaining a last resort. Pain medications usually fall into the first stage of treatment. If a patient takes maximum doses without relief, hormone therapy is next, as birth control pills, patches, and vaginal rings may offer symptom relief. Progestin therapy also proves helpful, as do a range of other drugs. Surgical removal of endometrial tissue may be done conventionally or laparoscopically. In extreme cases, hysterectomy may be necessary.
Fibroids
Fibroids Q & A
What causes fibroids?
The precise cause of fibroids is unknown, but genetic and hormonal factors may be contributory. Many fibroids have genetic changes that aren’t found in normal uterine tissue cells. Estrogen, progesterone, and some other hormones seem to encourage the growth of existing fibroids, and when hormones decrease after menopause, existing fibroids tend to shrink. Fibroids may grow quickly or slowly. They may stop growing at a certain size, or shrink on their own after a time. Fibroids present during a pregnancy may disappear or shrink afterward when the uterus returns to normal size.
What are the symptoms of fibroids?
Many cases of fibroids have no symptoms. Uterine fibroids aren’t usually dangerous unless they grow to abnormal sizes, because they’re benign and don’t turn cancerous. However, in some women, they do become symptomatic. When this occurs, common symptoms include:
- Periods lasting longer than a week
- Heavy menstrual bleeding
- Pain or pressure in the pelvis
- Urinary problems including frequent urination and difficulty emptying the bladder
- Backache and/or leg pains
- Constipation
Some types of fibroids may cause infertility, miscarriage, or complications during pregnancy.
How are fibroids treated?
Many cases of fibroids are of no consequence and require no treatment. Women with few or no symptoms may wish to watch and wait to see if fibroids grow in size or grow in impact.
For women who seek treatment, certain hormonal treatments may reduce problems with menstruation and may sometimes shrink the fibroids. Fibroids can be identified, located, and destroyed inside magnetic resonance imaging (MRI) scanners. There are also several laparoscopic surgical procedures that destroy fibroids within the body, as well as traditional surgical methods for their removal. Call or schedule an appointment online with the experienced and skilled physicians at Dr. Todd M. Goldberg. The practice is currently welcoming new patients and accepts most major forms of insurance.

STD Testing
STD Q & A
Is STD screening done during routine exams, such as Pap smears and blood tests?
Unless there are active symptoms that may stem from an STD, you’re probably not receiving any screening. If you feel you need these tests, request these from your caregiver. The type of screening you need depends on things such as age, sexual behavior, and other factors. The risk for various types of STDs changes depending on demographics and lifestyles.
Which STDs should I be tested for?
Chlamydia and gonorrhea testing should be done annually if you’re a sexually active woman under the age of 25. If you’re over 25, then these tests are only necessary if you’re engaged in elevated risk activities, such as with a new partner or with multiple partners. If your partner is a man who has had same-sex experiences, these tests are also advised.
The Center for Disease Control and Prevention encourages testing at least once for everyone between 15 and 65. High risk groups should be tested annually while actively involved in high-risk activities.
Hepatitis screening clears patients for vaccination for hepatitis A and B. People born between 1945 and 1965 should be tested for hepatitis C, since it’s high in that group and rarely shows symptoms until late stages. HIV and hepatitis are diagnosed by way of a blood sample.
Syphilis screening is recommended when you test positive for other STDs, have multiple partners, use intravenous drugs, or are pregnant or planning to be. Syphilis can be diagnosed through a blood test or a swab from genital sores, if these are present.
How is herpes screened?
There’s no reliable screening for herpes, which is a viral infection that may be passed on even if a person shows no symptoms. Testing tissue samples or culturing blister or ulcers may diagnose the infection, but even then, a negative result doesn’t rule out herpes. Blood tests may detect the condition, but these aren’t always reliable, since both false-positive and false-negative results are possible.

UTI
UTI Q & A
What is a UTI?
Any infection occurring in the urinary system — the kidneys through the ureters, to the bladder and urethra — comes under the UTI name. Most infections affect the lower tract, the bladder and urethra. While most lower UTIs are more annoying than dangerous, they can be quite painful. Should the UTI spread to the kidneys, however, the infection becomes much more serious. UTIs are treated easily in the early stages, and there are things a woman can do to reduce the chances of infection in the first place.
What are the symptoms of UTIs?
Not all UTIs display symptoms. When they do, these most commonly include:
- A persistent urge to urinate, while only producing a small amount
- Burning sensation when urinating
- Cloudy urine, or indications of blood, such as pink, red, or cola-colored urine
- Strong odors to the urine
- Pain, usually in the center of the pelvis
Each symptom may be a clue as to the type of UTI and the part of the urinary system that’s affected.
What causes UTIs?
UTIs usually occur when bacteria enter the urinary tract. The urinary system usually keeps these bacteria in check, but the system is occasionally overwhelmed and bacteria multiply to a level sufficient to cause infection. Bacteria may arrive via the digestive system, given the proximity between urethra and anus, but other bacteria may be introduced during sexual intercourse. Some UTIs stem from complications of sexually-transmitted infections as well.
How can I avoid UTIs in the first place?
There are things you can do to ease symptoms as well as avoid being infected in the first place. Drinking lots of water dilutes your urine and keeps the urinary system flushed out and functioning.
When you do have a UTI, lots of water remains a good idea. As well, avoid alcohol, caffeine and citrus, which can irritate the bladder and increase burning sensations when you urinate. While the evidence is mixed, some studies indicate that cranberry juice may help prevent UTIs, especially in women who suffer recurrent infections. It does have some drug interactions, so check with the doctor before drinking cranberry juice, especially if you’re using blood thinners or other prescription medications.
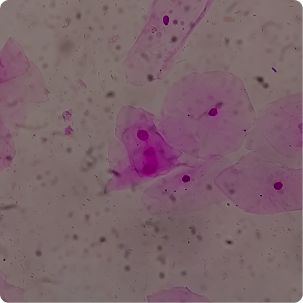
BV
BV Q & A
What causes BV?
There are both “good” and “bad” bacteria that exist in the vagina at any time. The good bacteria called Lactobacilli hold the anaerobes, the bad bacteria, in balance. When this balance is lost and anaerobes dominate, bacterial vaginosis develops.
Though it’s not fully understood why, BV often occurs when a woman has a new sex partner. Multiple and same-sex partners also seem to carry increased risk for BV. Douching may also precipitate an upset of bacterial balance, and this risk increases in women who douche more often. The vagina has its own cleaning system, so excess douching isn’t necessary. Some women naturally lack sufficient lactobacilli and are more prone to BV.
What symptoms does BV create?
Some women show few or no BV symptoms. In others, it may be hard to miss. Common symptoms include:
- Vaginal discharge that’s usually thin and colored gray, white, or green
- A strong odor usually described as fish-like
- Itching sensations in the vagina
- Burning sensations while urinating
It’s time to contact your caregiver about your symptoms if:
- You have a new vaginal discharge accompanied by a fever or strong odor
- You’ve previously had vaginal infections, but the discharge is different
- You’ve got a new partner or multiple partners, since BV may resemble symptoms from sexually transmitted infections
- Over-the-counter yeast infection treatments don’t work
How is BV treated?
Three medications are typically used to clear up BV. Metronidazole comes in pill form or as a gel administered vaginally. Clindamycin cream is also used in the vagina. Note that it may weaken latex condoms during and shortly after the treatment period. Tinidazole is an oral medication that works much like metronidazole. Both oral drugs may cause stomach upset and nausea, and patients should avoid alcohol while taking all of these medications.
Completing the full, prescribed course of medication is key to preventing recurrence, even if symptoms subside before the treatment period ends. It’s common for BV to reoccur, despite effective treatment. There may be some benefit to eating foods with lactobacilli, such as probiotic yogurts, but research is not yet conclusive.
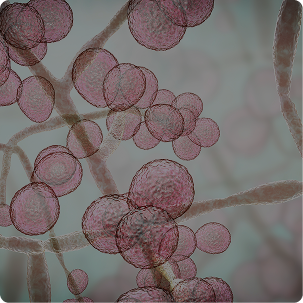
Yeast Infections
Yeast Infections Q & A
How do I know if I have a yeast infection?
Yeast infections range from mild to moderate, with symptoms that include:
- Irritation and itching of the vagina and vulva
- Burning sensation during urination or sexual intercourse
- Pain or soreness in the vagina
- A vaginal rash
- Redness and swelling of the vulva
- Odorless vaginal discharge that’s either watery or thick and white like cottage cheese
Complicated yeast infections often display multiple symptoms or these conditions:
- Severe redness, swelling, or itchiness that leads to sores, tears, or fissures
- 4 or more infections a year
- The patient is pregnant, or has diabetes or an immune system disorder
What causes yeast infections?
Yeast infections start with an overgrowth of a fungus called candida, which usually exists in balance with other yeasts and bacteria in the vagina. Normally, lactobacillus bacteria produce enough acid to keep candida in check, but when it doesn’t, candida overgrows and a yeast infection results. Some causes of yeast overgrowth are:
- Pregnancy
- Antibiotic use, which changes the acid balance in the vagina
- Diabetes, particularly when it’s uncontrolled
- Estrogen therapy or oral contraceptives
- Immune system problems
How are yeast infections treated?
Treatment varies for simple and complicated yeast infection cases. Over-the-counter and prescription antifungal medications can be administered over 1, 3, or 7 days, depending on the product, and may be enough to treat uncomplicated yeast infections. These medications may be available as a tablet, ointment, cream, or suppository. Some products may cause slight burning or irritation upon application, and since suppositories and creams are oil-based, users of latex-based condoms and diaphragms need to use alternate birth control methods during yeast infection treatment.
Complicated yeast infections require longer courses of treatment, typically 7-14 days in length. Fluconazole, effective as a single oral dose for simple infections, may be extended to 2 or 3 doses for complicated problems, but isn’t suitable for use during pregnancy. A yeast infection maintenance plan is possible for extreme cases.

Menorrhagia
Menorrhagia Q & A
What conditions define menorrhagia?
Menstrual bleeding is considered heavier than normal when one or more of the following conditions occur:
- Using one or more tampons or sanitary pad every hour for several hours
- The need to double up on sanitary protection to control menstrual bleeding
- Waking up in the night to change pads or tampons
- Periods of bleeding lasting more than a week
- Passing blood clots more than one day of the period
- Anemia, typically indicated by tiredness, fatigue, and shortness of breath
What causes menorrhagia?
Common conditions that give rise to menorrhagia include:
- Blood coagulation disorders
- Complications with pregnancy
- Hormone imbalances between estrogen and progesterone
- Medical conditions such as pelvic inflammatory disease, endometriosis, and thyroid problems
- Non-hormonal IUDs
- Ovary dysfunction: if ovulation doesn’t occur, no progesterone is produced and an imbalance occurs
- Some medications, including anti-inflammatories and anticoagulants
- Uterine fibroids or polyps
How is menorrhagia treated?
Treatment is based on what’s causing the problem as well as an assessment of the patient’s health. Drug therapy solutions include:
- Nonsteroidal anti-inflammatory drugs, or NSAIDs, help reduce menstrual blood flow with the added benefit of pain relief
- Oral contraceptives regulate the menstrual cycle and may reduce prolonged or excessive bleeding
- Oral progesterone may be helpful to restore hormone balance, which may stop menorrhagia
- An intrauterine device that releases progestin
- Tranexamic acid, a medication that helps decrease the blood loss
- Iron supplements may offset the symptoms or onset of anemia
Surgical treatments of menorrhagia include:
- Dilation and curettage
- Ultrasound ablation to shrink fibroids, if they’re causing the bleeding
- Endometrial ablation
- Uterine artery embolization
- Hysterectomy
When menorrhagia results from another condition, such as thyroid disease, treating the precipitating condition usually reduces menstrual blood flow. Call or schedule an appointment online.
Telephone
Patient Feedback
Celia Q.
“I have Dr. Goldberg as my doctor for so many years. My 2 daughters are also under his great care! I am so appreciative of the respect Dr. Goldberg gives to my questions, and the time and attention he gives to me. Really recommend him!”
Sheri T.
“I’ve been a patient of Dr. Goldberg for over two decades. He and his staff have consistently demonstrated exceptional kindness and professionalism. Visiting the OB/GYN clinic can be an uncomfortable experience, but Dr. Goldberg’s gentle and calming demeanor always puts me at ease. I genuinely appreciate all the doctors, nurses, and office staff at his practice.”
Maria C.
“Dr. Goldberg took the time to listen to my concerns and answered all my questions with patience and clarity. His knowledge and expertise were evident, and he provided recommendations tailored specifically to my health needs. I appreciated his compassionate approach, which made me feel comfortable.”



